Abstract
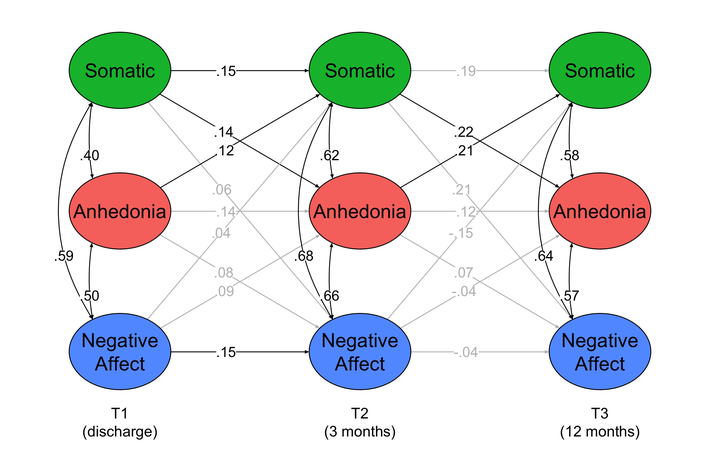
Background: Post-stroke depressive symptoms are prevalent and impairing, and elucidating their course and risk factors is critical for reducing their public health burden. Previous studies have examined the course of post-stroke depression, but distinct depressive symptom dimensions (eg, somatic symptoms, negative affect [eg, sadness], anhedonia [eg, loss of interest]) may vary differently over time. Objective: The present study examined within-person and between-person associations between depressive symptom dimensions across 3 timepoints in the year following discharge from in-patient rehabilitation hospitals, as well as the impact of multiple clinical variables (eg, aphasia). Methods: Stroke survivors completed the Center for Epidemiologic Depression Scale (CES-D) at discharge from post-stroke rehabilitation (“T1”) and at 3-month (“T2”) and 12-month (“T3”) follow-ups. Scores on previously identified CES-D subscales (somatic symptoms, anhedonia, and negative affect) were calculated at each timepoint. Random intercept cross-lagged panel model analysis examined associations between symptom dimensions while disaggregating within-person and between-person effects. Results: There were reciprocal, within-person associations between somatic symptoms and anhedonia from T1 to T2 and from T2 to T3. Neither dimension was predictive of, or predicted by negative affect. Conclusions: The reciprocal associations between somatic symptoms and anhedonia may reflect a “vicious cycle,” and suggest these 2 symptom dimensions may be useful indicators of risk and/or intervention targets. Regularly assessing depression symptoms starting during inpatient rehabilitation may help identify stroke survivors at risk for depression symptoms and facilitate early intervention.